Myofascial pain syndrome, a condition characterized by the presence of trigger points (TrPs) in muscles, has prompted various needling treatments. Among them, dry needling stands out as a popular approach in certain health care professions. This technique involves the skilled use of thin filiform needles to penetrate the skin, stimulating myofascial trigger points, musculature, and connective tissue for managing neuromusculoskeletal disorders. Unlike wet needling, which includes injections, dry needling does not introduce any substances into the trigger point area. This blog post delves into the clinical application, safety considerations, and effectiveness of dry needling in addressing myofascial pain.
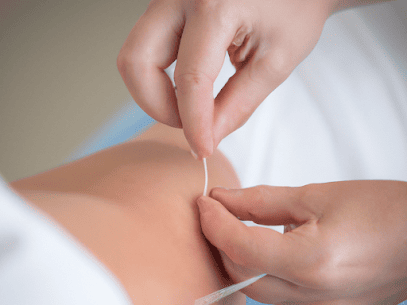
Understanding Dry Needling
The American Physical Therapy Association (APTA) defines dry needling as a skilled intervention that uses thin filiform needles to penetrate the skin, stimulating myofascial trigger points, muscles, and connective tissue for managing neuromusculoskeletal disorders. Similarly, the Australian Society of Acupuncture Physiotherapists describes it as a rapid, short-term needling approach to altered or dysfunctional tissues, aiming to improve or restore function. This may involve needling of myofascial trigger points, periosteum, and connective tissues.
Dry needling, often combined with electrical current to create modalities like electrical dry needling or percutaneous electrolysis, has gained popularity. In comparison to other needling therapies, such as injections or acupuncture, the current paper focuses on the rationale for the clinical application of dry needling for myofascial pain.
Clinical Application: The Local Twitch Response
A widely adopted needling approach for managing trigger points is the “fast in, fast out” method described by Hong. This technique entails inserting the needle into the trigger point until the first local twitch response is elicited. The local twitch response involves a brief and sudden contraction of a trigger point taut band, linked to the sensitivity of dysfunctional motor endplates.
Research by Hong suggests that needle penetration resulting in local twitch responses is more likely to lead to subsequent pain relief than needle penetration without such responses, regardless of the introduction of substances. However, the number of local twitch responses needed for a positive outcome has been a subject of debate.
Patients often perceive the local twitch response as an uncomfortable sensation during treatment. Clinicians must communicate this possibility to patients before the procedure, cautioning that needle contact with a trigger point may cause muscle twitching or a distant flash of pain. Some clinicians propose using referred pain, in addition to or instead of the local twitch response, during dry needling. Referred pain, when elicited during the clinical examination of a trigger point, can be monitored during the needling procedure.
Adverse Events and Safety
Clinicians practicing dry needling must adhere to guidelines for safe practice. The needle is considered an extension of the clinician’s finger, emphasizing the importance of proper identification of the trigger point area before insertion. Deep knowledge of human anatomy and the patient’s clinical status is crucial for minimizing adverse events.
While the risk of adverse events is generally small when experienced clinicians apply needling therapies, cases of significant complications, such as pneumothorax, puncturing the stomach, cardiac tamponade, epidural hematoma, hemiplegia, or infection, have been documented. Proper training and caution are imperative to mitigate potential serious complications associated with needling therapies.
Post-Needling Induced-Pain or Soreness
Patients undergoing dry needling are often advised about the potential presence of soreness after the procedure, termed post-needling induced-pain or soreness. This common minor adverse event can impact patient satisfaction and treatment adherence. Post-needling soreness is thought to result from neuromuscular damage generated by consecutive needling insertions into the muscle.
Clinicians employ various treatment modalities after dry needling to reduce post-needling induced pain. These may include postural education, activity modification, self-stretch, therapeutic exercise, or neuromotor re-training. Incorporating active therapies after the application of passive modalities, such as dry needling, aims to enhance the patient’s conscious awareness of normal muscle function and support the brainstem in incorporating restored full-range capability into daily activities.
Clinical observations suggest that patients typically recover from post-needling induced pain or soreness between 48 and 72 hours after the intervention. Studies investigating post-needling techniques, such as spray and stretch, ischemic compression, or low-load eccentric exercise, have shown effectiveness in reducing post-needling induced pain.
Effectiveness of Dry Needling
Dry needling for myofascial pain management was first reported 40 years ago, and since then, numerous clinical trials and systematic reviews have explored its effectiveness. However, there is no consensus regarding the superiority of dry needling over other needling therapies like injections.
Meta-analyses comparing wet needling (lidocaine injections) and dry needling for neck/shoulder myofascial pain suggest similar effectiveness with no clear differences between the two. The Canadian Agency for Drugs and Technologies in Health accepted the use of dry needling in the public health system in 2016, based on its effectiveness for musculoskeletal pain syndromes.
Research has investigated dry needling’s effectiveness for various conditions, including temporomandibular disorders, tension-type headache, shoulder pain, low back pain, and plantar heel pain. Meta-analyses and clinical trials have provided varying levels of evidence, with some supporting the effectiveness of dry needling for specific conditions and others yielding inconclusive results.
In conclusion, dry needling has become a widely used intervention for managing myofascial pain, with its effectiveness supported by some studies and clinical observations. However, ongoing research, proper training, and careful consideration of safety protocols are essential for advancing our understanding and ensuring the safe and effective application of dry needling in clinical practice.

